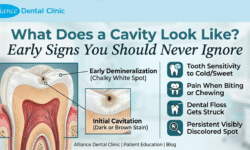
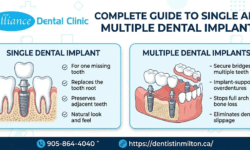
You notice it first as a dull ache at the very back of your jaw — maybe a little tenderness when you chew, some swelling near your gum line, or a throbbing pressure that radiates toward your ear. Now you are wondering: is this wisdom tooth pain, and how serious is it?
The answer matters more than most people realise. Wisdom tooth pain is not always a passing nuisance. Without proper evaluation, it can progress into infection, damage to neighbouring teeth, or complications that require far more involved treatment than a straightforward extraction. The good news is that catching problems early keeps treatment simple, fast, and far less expensive.
In this complete guide, written by the clinical team at Alliance Dental Clinic in Milton, we cover everything you need to know: what wisdom tooth pain actually feels like, whether everyone gets wisdom teeth, when extraction is necessary, what to expect during a wisdom tooth extraction, how to heal well afterward, and how to recognise a serious infection before it becomes a dental emergency.
What Is Wisdom Tooth Pain?
Wisdom tooth pain is the discomfort that occurs when your third molars — the last teeth to develop at the very back of the upper and lower jaw — begin pushing through the gum line. These teeth typically emerge between the ages of 17 and 25, though eruption can occur later in some adults.
Because the jaw has often already reached its full size by the time wisdom teeth arrive, there is frequently insufficient space for them to emerge correctly. This crowding causes pressure on the surrounding gum, bone, and neighbouring teeth — and that pressure is what most patients feel as wisdom tooth pain.
Pain intensity varies significantly. Some patients experience only mild, intermittent discomfort over a few days as the tooth breaks through the gum. Others develop persistent, severe throbbing that radiates toward the ear, neck, or temple and makes it difficult to eat, sleep, or concentrate. If your pain falls into the latter category, it is a signal that something beyond normal eruption is happening — and a prompt dental assessment is essential.
Wisdom Tooth Pain Symptoms: What to Look For
Based on what we see in practice every day at Alliance Dental Clinic Milton, here are the most common symptoms patients report before presenting for a wisdom tooth assessment:
- Throbbing ache at the far back of the upper or lower jaw, often worse at night
- Swollen, red, or tender gum tissue at the back of the mouth
- Pain or stiffness when opening the mouth or chewing
- Persistent headache or earache on the affected side
- Bad taste in the mouth or persistent bad breath not resolved by brushing
- Tender or swollen lymph nodes beneath the jaw
- Visible swelling along the cheek or jaw line
If you are experiencing several of these symptoms simultaneously — especially if fever is involved — this may indicate a wisdom tooth infection rather than straightforward eruption discomfort. Do not wait. Contact Alliance Dental Clinic for same-day emergency dental care in Milton.
Will Everyone Have Wisdom Teeth?
One of the questions we are asked most frequently during consultations: “Will everyone have wisdom teeth?” The answer is no — not by a long way.
Most adults develop between one and four wisdom teeth. However, research published in peer-reviewed dental literature estimates that approximately 35% of people are born without any wisdom teeth at all. This is a genuine evolutionary trait. As modern human diets changed over thousands of years and jaws became smaller, the third molar became increasingly redundant. Some populations show even higher rates of wisdom tooth absence — studies of certain Indigenous populations and East Asian groups have found rates exceeding 40%.
Whether you develop wisdom teeth, how many you develop, and how they are positioned are all largely determined by genetics. If your parents had problems with their wisdom teeth, there is a meaningful chance you may too.
The only reliable way to confirm whether you have wisdom teeth developing — and what they are doing beneath the surface — is through a dental X-ray. At Alliance Dental Clinic in Milton, our routine preventive dental examinations include digital radiography specifically designed for early detection of developing wisdom teeth, long before they cause symptoms or problems.
Why Are Wisdom Teeth Taken Out?
Understanding why wisdom teeth are taken out helps patients make informed decisions rather than simply deferring to the dentist’s recommendation without context. Here is what the clinical evidence and our practical experience tell us.
Not every wisdom tooth needs to be removed. A wisdom tooth that erupts fully, aligns correctly with the opposing teeth, and can be effectively cleaned with a toothbrush and floss is considered a functioning tooth. It can be monitored and left in place. The problem is that this ideal scenario represents a minority of cases. Most patients do not have sufficient jaw space for wisdom teeth to erupt without complications.
Clinical Reasons for Wisdom Teeth Removal
- Impaction: The tooth is partially or fully trapped beneath the gum or jawbone. Impacted wisdom teeth are the most common source of chronic wisdom tooth pain and can cause progressive damage to adjacent teeth and surrounding bone. The Canadian Dental Association (CDA) recognises impaction as one of the primary clinical indications for extraction.
- Pericoronitis: When a wisdom tooth partially erupts, the gum flap covering it creates a pocket where bacteria and food debris accumulate. This causes a painful, recurring infection known as pericoronitis. Left unaddressed, pericoronitis can spread to surrounding tissue and become serious.
- Crowding and bite disruption: Emerging wisdom teeth exert lateral pressure on neighbouring molars, shifting the bite and potentially reversing orthodontic treatment. This is particularly relevant for patients who have had braces.
- Dental decay: Wisdom teeth sit so far back in the mouth that effective cleaning with a toothbrush is extremely difficult. Cavities in wisdom teeth are disproportionately common and tend to progress faster due to the inaccessibility of the area.
- Cysts and pathology: An impacted wisdom tooth can develop a dentigerous cyst around its crown. These fluid-filled sacs gradually destroy surrounding bone, damage neighbouring tooth roots, and may eventually require more extensive surgical treatment if ignored.
- Accelerated gum disease: The deep pockets that form around partially erupted or impacted wisdom teeth create ideal conditions for the bacteria responsible for periodontal (gum) disease.
At Alliance Dental Clinic Milton, we review each patient’s X-rays and clinical presentation individually. We recommend wisdom tooth extraction only when it is in the patient’s clear long-term interest — never as a routine procedure performed without clinical justification.
Dry Socket After Wisdom Tooth Extraction: What It Is and How to Prevent It
Dry socket is one of the most common complications following a wisdom tooth extraction, and knowing what it is gives you a significant advantage in preventing and recognising it early.
After a wisdom extraction, the body forms a blood clot inside the empty socket. This clot serves a critical function: it covers and protects the exposed bone and nerve endings while the underlying tissue heals. Dry socket — medically called alveolar osteitis — occurs when this clot is dislodged, dissolves prematurely, or fails to form correctly. Without the clot, bone and nerve tissue are left exposed to air, food, and bacteria.
Dry socket is not just uncomfortable — it is genuinely painful. Many patients describe it as significantly worse than the original tooth pain that prompted extraction in the first place.
How Common Is Dry Socket?
According to clinical data, dry socket affects approximately 2–5% of all tooth extractions. However, for lower wisdom tooth extractions specifically, rates can reach as high as 30%. Risk is elevated in smokers, patients on hormonal contraceptives, those with poor blood supply to the jaw, and patients who do not follow post-operative instructions carefully.
Signs and Symptoms of Dry Socket
- Intense, throbbing pain beginning 3–5 days after extraction — noticeably worsening rather than improving
- Pain radiating toward the ear, eye, temple, or neck on the same side as the extraction
- A visibly empty socket where a dark blood clot should be visible
- Persistent bad taste or bad breath that does not resolve with gentle rinsing
- Visible bone inside the socket
If you recognise these signs following a wisdom extraction in Milton, call Alliance Dental Clinic immediately. Dry socket is treated quickly and effectively in-clinic with a medicated dressing placed directly into the socket. Most patients experience significant pain relief within hours of treatment.
How to Prevent Dry Socket
- No straws for 72 hours minimum — the negative suction pressure can dislodge the forming clot
- No smoking or tobacco use for at least 48–72 hours; ideally longer — nicotine and the physical act of inhaling both significantly increase dry socket risk
- Soft diet only for the first 3–5 days — yogurt, mashed potatoes, broth, smoothies consumed with a spoon
- No vigorous rinsing for 24 hours; begin gentle warm salt water rinses only after the first day
- Avoid strenuous physical activity for 48 hours — elevated heart rate and blood pressure can disrupt clot formation
- Do not probe the socket with your tongue, fingers, or any implement
The Wisdom Tooth Extraction Process: A Step-by-Step Guide
Dental anxiety is one of the most common reasons patients delay seeking care for wisdom tooth pain — and it is often the fear of the unknown rather than the procedure itself that causes the most distress. At Alliance Dental Clinic in Milton, we believe informed patients have better experiences. Here is exactly what happens during a wisdom tooth extraction at our clinic.
Step 1: Consultation and Diagnostic Imaging
Before any extraction is scheduled, we conduct a thorough clinical examination and take digital X-rays or a panoramic radiograph. This allows us to assess the exact position, depth, angle, and root formation of your wisdom teeth and confirm whether a simple extraction or a surgical approach is required. We use this stage to answer all your questions and ensure there are no surprises on the day of the procedure.
Step 2: Anaesthesia and Comfort Measures
Local anaesthesia is administered to fully numb the treatment area. You will not feel pain during the procedure — only pressure, vibration, or movement, which are normal sensations during extraction. For patients with significant dental anxiety, sedation options are available. Please let us know when booking so we can arrange the most comfortable option for you.
Step 3: Simple Extraction
If the wisdom tooth has fully erupted and is accessible, a simple extraction is performed. The dentist uses specialised elevators to gently widen the socket and loosen the periodontal ligament — the tissue connecting the tooth to the bone — before carefully removing the tooth. This typically takes only a few minutes per tooth.
Step 4: Surgical Extraction (for Impacted Teeth)
Impacted or partially erupted wisdom teeth require a surgical approach. A small, precise incision is made in the gum tissue to expose the tooth. In some cases, a small amount of bone covering the tooth is removed. The tooth may be sectioned — cut into two or three pieces — to allow controlled removal with minimal trauma to the surrounding area. This sounds more alarming than it feels; you remain comfortable throughout.
Step 5: Cleaning, Stitching, and Immediate Recovery
The socket is irrigated and thoroughly cleaned after the tooth is removed. Dissolvable sutures are placed where needed to encourage proper healing. Gauze is placed over the socket to manage initial bleeding. Before you leave, our team provides written post-operative instructions and is available to answer any questions that arise during your recovery at home. Most complete wisdom extraction procedures take between 20 and 60 minutes depending on complexity.
Healing After Wisdom Tooth Extraction: A Day-by-Day Guide
How well an extracted wisdom tooth heals depends heavily on what you do in the first few days after the procedure. This section draws directly on the post-operative protocols we use at Alliance Dental Clinic Milton to support our patients through a smooth, complication-free recovery.
First 24 Hours — Rest and Protection
This is the most critical window. The blood clot that will protect your socket forms in these first hours. Rest completely. Bite gently but firmly on the gauze pad. Change gauze as directed — typically every 30–45 minutes until bleeding slows to a light ooze. Apply an ice pack to the outside of the cheek in 20-minute cycles to reduce initial swelling. Do not rinse, spit forcefully, smoke, drink through a straw, or disturb the socket with your tongue or fingers.
Days 2 and 3 — Peak Swelling
Swelling typically peaks at 48 hours before gradually subsiding. Some bruising on the cheek and jaw is normal. Begin gentle warm salt water rinses (one teaspoon of salt dissolved in a glass of warm water) after the first 24 hours. Take prescribed or recommended pain relief as directed. Pain should be manageable and should show some improvement each day. If it is worsening, contact us.
Days 4–7 — Gradual Improvement
Most patients notice significant improvement in comfort and jaw mobility by day 4–5. Dissolvable stitches may begin to loosen. Continue salt water rinses. You can gradually reintroduce slightly firmer foods such as scrambled eggs, soft pasta, and well-cooked vegetables. Avoid hard, crunchy, chewy, or spicy foods until the socket has visibly closed.
Weeks 2–4 — Gum Closure
Gum tissue closes over the socket surface during this period. You can generally return to a completely normal diet. Deep bone healing continues beneath the surface for several months — this process is painless and unnoticeable in daily life.
What Normal Healing Looks Like
- Dark red or maroon blood clot visible in the socket within the first 24 hours
- Mild to moderate swelling and possible light bruising on the cheek and jaw
- White or cream-coloured tissue in the socket after the first few days — this is healthy granulation tissue, not infection or pus
- Pain that decreases steadily day by day
When to Call Alliance Dental Clinic Immediately
- Severe, worsening pain 3–5 days post-extraction — possible dry socket
- Fever above 38°C (100.4°F)
- Persistent heavy bleeding not controlled by gauze pressure after 45 minutes
- Swelling that is increasing rather than decreasing after 72 hours
- Difficulty swallowing or any sense of throat tightness
- Prolonged numbness or tingling beyond a few hours post-anaesthesia
Wisdom Tooth Infection: Recognising and Acting on a Serious Complication
A wisdom tooth infection is among the most serious dental complications we encounter at Alliance Dental Clinic. Unlike straightforward eruption pain — which is uncomfortable but not dangerous — a dental infection can escalate rapidly and, in severe cases, become life-threatening if it spreads to the airway or bloodstream.
Infections associated with wisdom teeth arise in three main clinical contexts: pericoronitis (infection of the gum flap around a partially erupted tooth), pulp infection from advanced decay inside the wisdom tooth, and post-extraction socket infection following a wisdom removal.
Symptoms of a Wisdom Tooth Infection
- Persistent, throbbing pain spreading toward the jaw, ear, or throat
- Visible swelling of the face, cheek, or along the jaw line
- Difficulty opening the mouth, chewing, or swallowing
- Fever, chills, and a general feeling of systemic illness
- Pus or discharge around the tooth or socket
- A foul, persistent taste in the mouth
- Tender, swollen lymph nodes under the jaw or in the neck
Critical warning: If you develop facial swelling that is spreading, difficulty breathing or swallowing, or a high fever alongside tooth pain, this constitutes a dental emergency. Go to the nearest emergency department or call emergency services immediately, in addition to contacting your dentist. These symptoms can indicate Ludwig’s angina or another spreading deep-space infection that requires urgent medical attention beyond routine dental care.
How a Wisdom Tooth Infection Is Treated
Treatment depends on the severity and stage of the infection. In most cases, the approach at Alliance Dental Clinic Milton involves a prescribed course of antibiotics to control the active infection, followed by wisdom tooth extraction once the acute phase has resolved. Attempting to extract a severely infected tooth at the height of infection carries additional risks, which is why we stage treatment appropriately. In cases where an abscess has formed, drainage may be performed as part of the initial appointment.
Dental infections do not resolve on their own. Without treatment, they will worsen and spread. If you suspect a wisdom tooth infection in Milton, do not delay — call Alliance Dental Clinic for a same-day emergency appointment.
Why Choose Alliance Dental Clinic for Wisdom Tooth Extraction in Milton?
Alliance Dental Clinic has been serving Milton and the surrounding community for years, providing gentle, evidence-based dental care to patients of all ages. Here is what sets our approach to wisdom teeth removal apart:
- Clinical expertise: Our dental team performs both simple and surgical wisdom tooth extractions, including cases involving deeply impacted or angulated teeth.
- Advanced digital imaging: We use low-dose digital radiography for accurate pre-surgical assessment and planning, minimising radiation exposure while maximising diagnostic quality.
- Pain-free approach: We use modern local anaesthesia protocols and offer sedation options for anxious patients so that every extraction is as comfortable as possible.
- Transparent pricing: We always provide a clear, itemised cost estimate before any procedure begins. We help patients navigate insurance coverage and offer flexible payment options.
- Emergency availability: We offer same-day emergency appointments for patients experiencing severe wisdom tooth pain or signs of infection.
- Continuity of care: From initial assessment through to healing check-ups, your care is managed by a consistent, familiar team who knows your history.
Concerned About Wisdom Tooth Pain in Milton?
Whether you are experiencing your first twinge of discomfort at the back of the jaw or are dealing with significant swelling and pain, the team at Alliance Dental Clinic is here to help. Early evaluation makes everything simpler — and significantly reduces the risk of complications developing. Do not wait for pain to intensify before seeking care. Schedule a comprehensive dental examination today.
Frequently Asked Questions About Wisdom Teeth
What does wisdom tooth pain feel like?
Wisdom tooth pain typically presents as a dull, persistent ache or a sharp throbbing sensation at the far back of the upper or lower jaw. It frequently radiates toward the ear, neck, or temple on the affected side. The nature and severity of pain depends on whether the tooth is simply erupting, impacted, partially erupted, or infected.
Will everyone have wisdom teeth?
No. Approximately 35% of people never develop wisdom teeth at all, and many others develop fewer than four. A dental X-ray is the only reliable way to confirm whether wisdom teeth are present and what they are doing beneath the gum line. At Alliance Dental Clinic Milton, we check for wisdom tooth development as part of routine preventive examinations.
Do you have to remove wisdom teeth?
Not always. Wisdom teeth that erupt fully, align correctly, and can be cleaned effectively may be monitored and left in place. However, most patients do not have sufficient jaw space for wisdom teeth to emerge without causing problems. Your dentist will assess your specific situation with X-rays and only recommend wisdom teeth removal when there is a clear clinical indication.
How painful is wisdom tooth extraction?
The extraction itself should be entirely pain-free. Local anaesthesia numbs the area completely, so you feel pressure and movement but not sharp pain. Post-operative discomfort is manageable with over-the-counter analgesics in most cases, and prescription pain relief is provided where needed. Sedation is available for patients with significant dental anxiety. Most patients tell us the procedure was far less uncomfortable than they expected.
Can a wisdom tooth infection go away on its own?
No. Dental infections do not self-resolve and typically worsen progressively without treatment. Antibiotics can control the spread of infection, but they do not eliminate its source — the problematic tooth must still be treated or extracted. Never delay seeking professional care for a suspected dental infection. The Government of Canada’s oral health guidance emphasises that untreated dental infections carry serious health risks.
How much does wisdom tooth extraction cost in Milton?
The cost of wisdom tooth extraction in Milton at Alliance Dental Clinic varies depending on whether the procedure is a straightforward erupted extraction or a surgical extraction for an impacted tooth. We always provide a clear, upfront cost estimate before any procedure begins. Most dental insurance plans provide partial or full coverage for clinically necessary wisdom tooth removal. We also offer flexible payment arrangements. Call us at 905-864-4040 to discuss your specific situation and confirm your coverage before your appointment.
The Bottom Line
Wisdom tooth pain is one of the most common dental concerns our team encounters — and one of the most important not to ignore. Whether the discomfort stems from a tooth erupting in limited space, an impaction pressing against a neighbouring molar, or the early stages of a wisdom tooth infection, the principle is consistent: earlier care always means simpler, less invasive treatment and a lower risk of complications.
Do not wait for pain to become unbearable. Do not assume discomfort will pass on its own. Trust what your body is telling you, and trust a clinician who can give you answers based on your actual X-rays and clinical examination — not on generic online advice.
For trusted, patient-centred wisdom tooth care in Milton, visit Alliance Dental Clinic. Explore our complete range of dental services, or learn more about how we approach family dentistry for patients of all ages in Milton.